The gastric bypass was first performed many decades ago and quickly became the gold standard in bariatric surgery. This was due to the excellent safety profile, combined with very good long-term weight loss and disease improvement results. The gastric bypass, while not the most popular bariatric surgical procedure anymore, does offer exceptional benefits to many patients, especially those who suffer from uncontrolled diabetes or acid reflux.
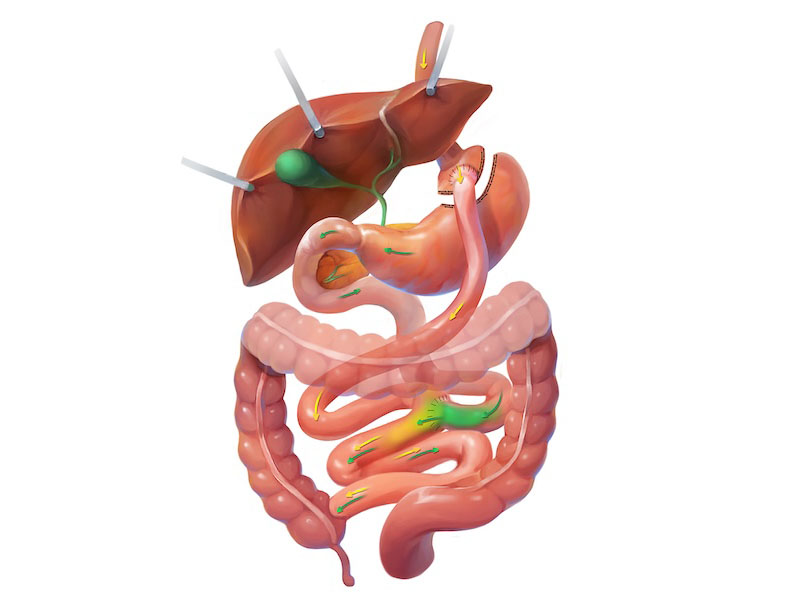
Gastric bypass is a two-part procedure with the first part being restrictive, mechanical reduction of the size of the stomach pouch. Dr. Higa will cut away approximately 85% of the stomach leaving a small pouch that approximates the size and volume of a golf ball. This becomes the new, primary receptacle for food. However, unlike the gastric sleeve, the portion of the stomach cut away during the gastric bypass is not removed from the abdomen and continues to produce and deliver gastric juices further down in the intestinal tract.
Once the new pouch has been created, Dr. Higa will bypass a portion of the small intestine to reduce the amount of intestinal surface area that food comes in contact with. This reduces the number of calories that can be absorbed into the body, adding yet another mechanism by which you can lose weight. Gastric juices and food take a separate track and meet at the Roux-en-Y further down the small intestine.
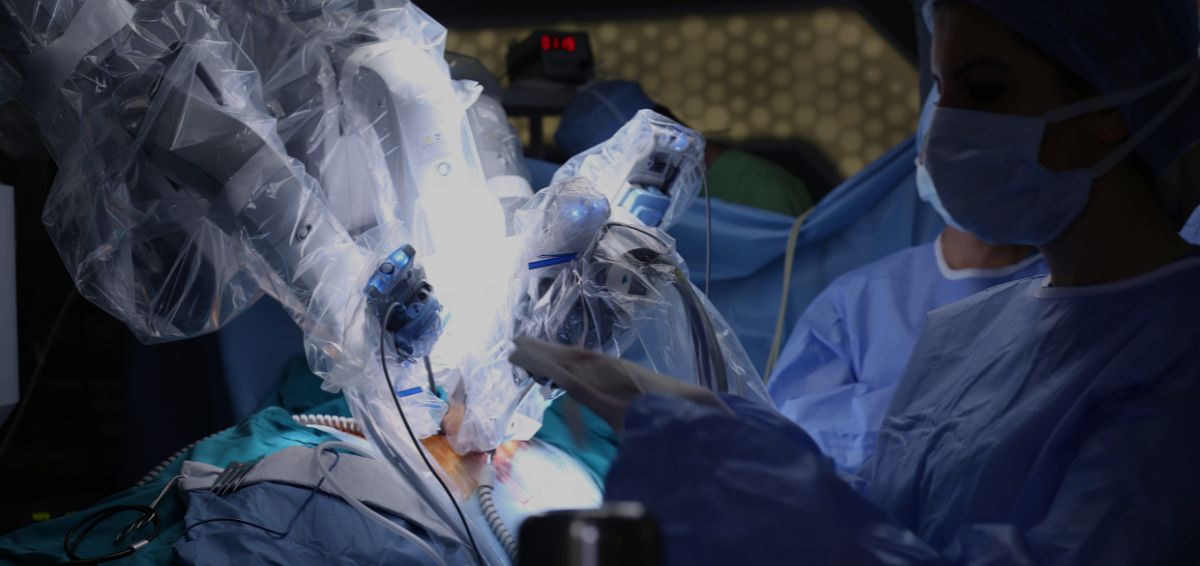
The gastric bypass is performed in a minimally invasive or laparoscopic manner. This requires only 4-5 small incisions in the abdomen. Dr. Higa also performs this procedure with the assistance of a surgical robot. This new technology allows for more precise movements within the abdomen and better visualization of the surgical field. Patients will be under general anesthesia for the procedure and the entire surgery takes about an hour to an hour and fifteen minutes.
Patients will then spend 1 to 2 nights in the hospital recovering before they are discharged home. While in recovery at the hospital, patients will be started on a clear liquid diet for the first several days after surgery. They will slowly progress through a range of diets, including full liquid, soft food, and modified solid food over the next several weeks.
If you are looking to pay for your procedure out of pocket, please visit our cash pay pricing.
To learn more about the gastric bypass, we encourage you to schedule a consultation with Dr. Higa. During this conversation you will learn more about how these benefits and risks may apply to your particular situation and, if indeed, the gastric bypass is right for you.
Use the contact form below to request an appointment