The gastric sleeve began as the second part of a two-part procedure known as a duodenal switch. The gastric sleeve was performed on extremely obese patients because it was seen as a safer primary-stage procedure before modifying the small intestine with the DS. However, as time went on, it became clear that the gastric sleeve had excellent results as a standalone procedure. This led to the gastric sleeve being considered, and ultimately approved, as a major bariatric option in and of itself.
Gastric sleeve surgery is currently the most popular bariatric surgical procedure in the United States. There is a very good reason for this popularity – its simplicity. It is both a straightforward procedure, but also a very effective one.
The gastric sleeve is purely restrictive, meaning that it simply reduces the size of the stomach, limiting the number of calories that can be consumed at any given meal, unlike the gastric bypass which includes a malabsorptive component (bypassing the intestine).
But the gastric sleeve also provides a hormonal weight loss benefit. Due to the way the gastric sleeve is performed, ghrelin, a hunger hormone secreted from the fundus of the stomach, is significantly reduced, and most patients experience a reduction in hunger.
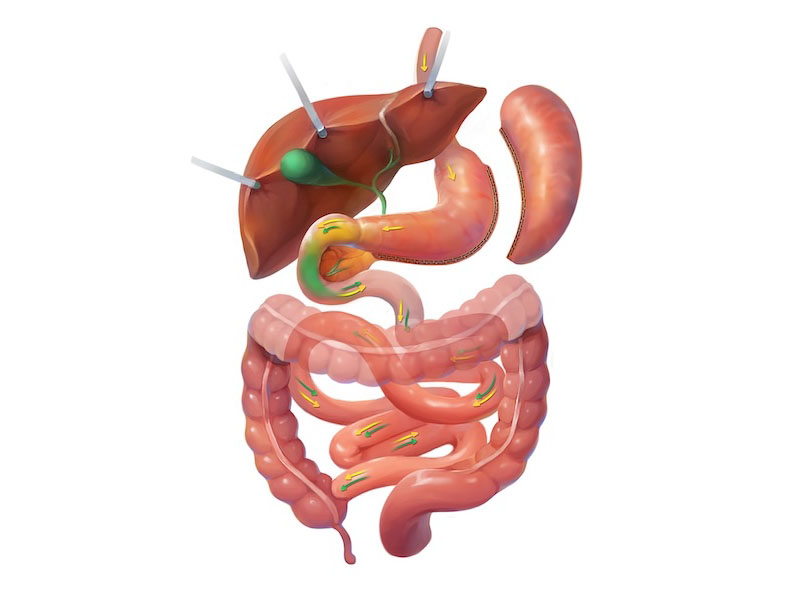
The sleeve is performed under general anesthesia and usually in a hospital setting. Four to five small incisions are made in the abdomen. This is known as laparoscopic, or minimally invasive, surgery and replaces traditional open surgery that requires a single, long incision to access the abdominal cavity. The abdomen is inflated with carbon dioxide gas to allow Dr. Higa enough space to perform the surgery. Then, specially-made medical devices are passed through trocars, which are used to protect the skin around the incision and act as passageways into the abdomen. If robotic surgery is employed, the robot is docked next to the patient and appropriate devices are attached to its arms.
Dr. Higa passes a device known as a French bougie through the throat and into the stomach. This allows him to accurately determine how much stomach should be cut away during the procedure. Using an advanced stapling device with multiple rows of staples, Dr. Higa will slowly separate the stomach in two. What remains is about a quarter of the size of the original stomach retaining the general shape of a sleeve or banana. The upper and lower parts of the GI tract are left untouched.
If you are looking to pay for your procedure out of pocket, please visit our cash pay pricing.
The gastric sleeve is a straightforward and effective procedure that not only offers excellent potential for weight loss but also has fantastic disease improvement and resolution results. Patients should know, however, that the gastric sleeve is not a magic bullet and, just like any procedure, requires a great deal of dedication from the patient to achieve the best results. To learn more about the gastric sleeve, we encourage you to watch our online seminar or to visit Dr. Higa for a consultation.